UNDERSTANDING SPINAL CORD INJURY (SCI)
OVERVIEW
The spinal cord is a thick bundle of nerves that connects the brain to the rest of the body. It acts like an information highway, sending messages back and forth. A spinal cord injury, or SCI, refers to damage to the spinal cord. This can lead to a loss of muscle movement, called paralysis, and a loss of sensation. It can also affect basic body functions like urination, blood pressure and breathing.
- Introduction
- The nervous system
- What Do I Need to Know?
- Types of spinal cord injury
- Understanding your injury level
- Understanding your injury: complete vs incomplete injuries
- What is Different Now?
- Physical effects of spinal cord injury
- What Can I Do?
- Who Can Help Me?
- List and description of spinal cord injury clinicians and supports
- Conclusion & Resources
- Information and further reading
INTRODUCTION
The nervous system
The spinal cord is a thick bundle of nerves that connects the brain to the rest of the body. It acts like an information highway, sending messages back and forth. The spinal cord allows us to move our muscles and feel sensations like touch and temperature that let us know what is happening in the world around us.
A spinal cord injury, or SCI, refers to damage to the spinal cord. When the spinal cord is damaged, the flow of information between the brain and the body is disrupted or completely cut-off. This can lead to a loss of muscle movement, called paralysis, and a loss of sensation. It can also affect basic body functions like blood pressure and breathing. Any nerves above the injury (toward the head) continue to work. Any nerves below the injury (toward the tailbone) can be affected. Damage to the spinal cord can happen due to traumatic injuries such as motor vehicle accidents, falls, and violence. They can also happen due to non-traumatic injuries such as cancer, inflammation, and lack of oxygen to the spinal cord.
Regardless of the cause it is important to note that the spinal cord is rarely severed by an injury, and the problem is not that the spinal cord is torn, but that it is bruised or scarred which affects the ability for messages to travel up and down the spinal cord properly. The cells of the brain and the spinal cord are different from those of the rest of the body; they do not seem to regenerate once they are damaged.
In the short term, a spinal cord injury is a medical emergency and requires expert treatment at a trauma centre. The initial treatment may include surgery, and is aimed at limiting the damage to the spinal cord and enhancing the potential for recovery. Once a person is medically stable, they can begin a program of rehabilitation, which is also called rehab. This begins while they are still at an acute care hospital, but most people will get the best outcome if they complete a program in a specialized spinal cord injury rehab centre such as GF Strong.
The long-term outcome of a spinal cord injury can be very difficult to predict. The one rule is that every injury is unique. Recovery of some movement or sensation may occur, especially during the weeks or months following an injury.
If you’ve experienced a spinal cord injury, what you need to know is that you will be able to live a full and healthy life, regardless of how much recovery you experience. To do so, you’ll need proper rehabilitation and good medical care, as well as equipment and other supports, and the right information. You will need to pay special attention to your body and learn new ways of taking care of yourself.
This website is a resource to help you understand how your body works after SCI and to learn the supports and tools to help you manage it.
DID YOU KNOW?
The spinal cord cannot heal itself in the way that damaged skin or bone will heal.
DID YOU KNOW?
After SCI, you will be able to live a full and healthy life, regardless of how much you recover.
WHAT DO I NEED TO KNOW?
Types of SCI
The effect of a spinal cord injury depends on the level of the spinal cord that is damaged, as well as the degree of damage. The injury can happen in your neck, back, or lower back. The higher the injury, the more parts of the body are likely to be affected. If the injury is at the level of you back or lower back, the muscles in your legs and possibly your trunk may be affected. When you experience paralysis in your lower body, this is called paraplegia. A higher injury, at the level of the neck, can affect the hands, arms & breathing muscles in addition to the trunk and legs. This is called quadriplegia or tetraplegia.
Understanding your injury: Levels of injury
Knowing the level of your injury is key in understanding what parts of the body might be affected by paralysis and loss of function. The most important, and sometimes frustrating thing to know is that each person’s recovery from spinal cord injury is different.
There are 33 bones called vertebrae that protect the spinal cord. They are labeled to indicate where they are located on the spine:
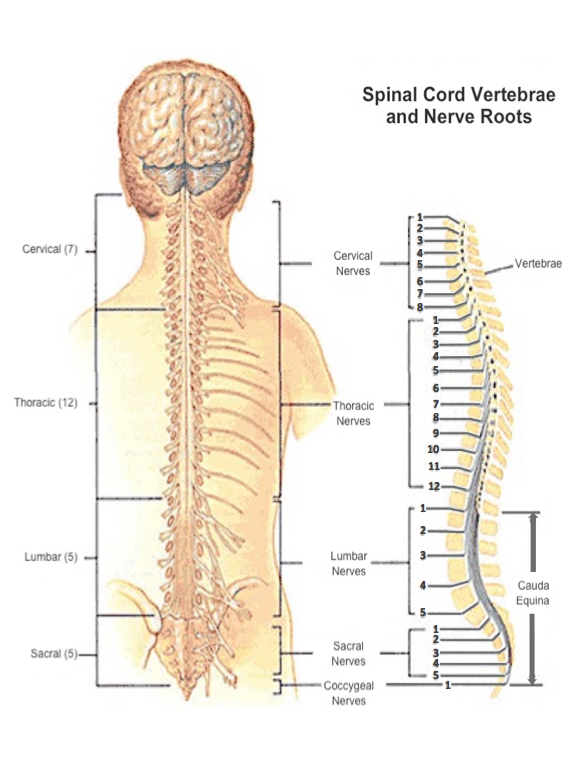
● C stands for cervical, or neck. There are 7 bones in the neck: C1 at the base of the skull through to C7 at the bottom of the neck. The nerves from the Cervical section of the spinal cord injury supply the neck, shoulders, arms and the diaphragm (the main breathing muscle).
● T stands for thoracic, or chest. There are the 12 bones in the back, located behind the rib cage: T1 at the top of the back through to T12 at the bottom. The nerves from the Thoracic section of the spinal cord supply the chest and abdominal muscles.
● L stands for lumbar, located in the lower back. There are 5 bones in this region. The nerves from the Lumbar section of the spinal cord supply the hips and legs.
● S stands for sacrum, which is the bone at the base of the spine. Technically this contains 5 vertebrae, but they are fused into a single bone. The nerves from the sacral section of the spinal cord control the pelvic organs such as the bladder, bowel and sex organs.
● Finally, there are 4 more bones fused together to make the coccyx, or tailbone.
The level of injury is identified by the lowest part of the spinal cord that functions normally. An injury to the neck area, for example at the C-6 level, can result in impairment to the arms, hands, trunk & legs, and can affect a person’s breathing muscles. A lower injury to the back, for example at the T10 level, can result in impairment mainly in the legs, with no impact on breathing or arm muscles.
Understanding your injury: Complete and Incomplete injuries
In some spinal cord injuries, the flow of information through the spinal cord is completely stopped. This is known as a complete spinal cord injury. In other injuries, some information is still able to pass through the injured area; this is known as an incomplete spinal cord injury. A common belief is that the spinal cord is either completely severed or partially severed to create an incomplete injury. In actual fact the spinal cord is rarely severed, and “completeness” of a spinal cord injury depends on whether there is any signal getting all the way to the bottom of the spinal cord.
It’s important to understand:
- The completeness of the injury depends on how many of the nerve pathways have been affected. If there is some signal getting through, then the injury is considered incomplete.
- The final test to see if a signal is getting to or from the brain to the very bottom of the spinal cord is done with a digital rectal exam. The nerves at the very bottom of the spinal cord are the nerves responsible for bladder, bowel and sexual function.
Many people use the term ‘complete’ to mean no sensation or movement below the level of injury, and the term ‘incomplete’ to mean some sensation or movement below the level of injury. The ASIA (American Spinal Injury Association) Standards are used by health professionals to determine if the injury is complete or incomplete. It uses an assessment tool called the ASIA Impairment Scale (AIS) to define all spinal cord injuries in the same way.
Complete Injury (AIS A)
With a complete SCI there is essentially no communication between the brain and the rest of the body below the injury. This is referred to as ASIA Impairment Scale (AIS) A.
Incomplete Injury (AIS B-E)
With an incomplete SCI, some messages to and from the brain below the level of injury are still able to get through. This means there may be some feeling or movement below the injury.
- AIS B: If there is any feeling or muscle activity in any part of the body below the injury, even if it is only in the rectum, the classification will be at least AIS B. This is often accompanied by some level of feeling in other parts of your body below the level of the injury.
- AIS C: Some weak movement below the level of the injury.
- AIS D: If the movement is stronger but still not normal.
- AIS E: Normal strength and sensation.
Each spinal cord injury is as unique as the person who experiences it. Your rehab team will make the most accurate prediction possible for your potential recovery, based on the level and type of your injury. Some people may recover sensation and the ability to move their muscles, and others may not. For those who do experience recovery, it’s difficult to predict how much they will recover or how long it will take.
DID YOU KNOW?
Understanding the level of your injury is key!
RESOURCE
What is a Spinal Cord Injury?
DID YOU KNOW?
The spinal cord is rarely completely severed! The completeness of the injury depends on how many of the nerve pathways have been affected.
RESOURCE
Complete vs. Incomplete
READ MORE
Five stories of Incomplete SCI from The Spin.

Image (c) International Collaboration on Repair Discoveries, C. Niamath, 2014.
WHAT’S DIFFERENT NOW?
Damage to the spinal cord interrupts the flow of messages between parts of the nervous system. This can affect the way your body works in three ways:
● First, you may experience changes in your ability to control the movement of your muscles in some parts of your body. You may experience paralysis, which means losing the ability to move a muscle, or muscle spasms, which are involuntary muscle movements known as spasticity.
● Second, you may experience changes in your sensation in some parts of your body. This can affect your senses of pressure, touch, temperature and pain;
● Finally, you may experience changes in certain special functions of the nervous system, called AUTONOMIC, that control basic body functions like blood pressure, temperature control and sweating.
Physical Effects
After a spinal cord injury, many people experience changes other than paralysis and loss of sensation.
Other effects may include:
- Loss of bowel and/or bladder control
- Changes in sexual function, sensitivity and fertility.
- Loss of the ability to feel heat, cold, touch and to regulate temperature
- Amplified reflex activities or spasms
- Pain or an intense sensation similar to pain
- Difficulty breathing, coughing or clearing secretions from your lungs
- Anyone with an injury above the T6 level needs to be aware of a dangerous condition called autonomic dysreflexia. Autonomic dysreflexia, AD, is an increase in blood pressure and signs include headaches, sweating and goose bumps.
Other impacts of SCI
- Spinal cord injury is an individual experience that affects the body, mind and soul.
- Speak to your social worker about how your injury is affecting you.
- Remember your resources can include psychologist, psychiatrist, spiritual care, peer support (SCI-BC) and community resources.
DID YOU KNOW?
Nothing you learn or develop in rehab will be wasted if your body continues to recover.
Never Say Never!
In rehab, we always hope for future recovery & we work with the function you have right now.
WHAT CAN I DO?
The best outcomes after spinal cord injury come when individuals who are injured participate fully in a specialized rehabilitation program. Your role is to be as actively involved in your rehabilitation as you can, and to learn about your specific injury and how it affects you.
For some it can be a struggle to accept that a spinal cord injury diagnosis isn’t reversible. As a result, some people are tempted to focus only on complete recovery, at the expense of participating fully in rehab. Most people only get one opportunity to attend rehab and learn the important skills and adaptations to help you live a full life at your current level of function. It’s important to remember that nothing you learn or develop in rehab will be wasted if your body recovers further. In fact, many therapies that you receive in rehab will assist you in understanding how much recovery is possible and allow you to do the most with what you have.
Rehabilitation is the process of maximizing your ability after a major injury – at a rehab centre, you will learn about your injury and how to teach others, learn about how to care for yourself post-SCI, and learn how to get back to living in your community.
WHO CAN HELP ME?
All clients/patients have a team of healthcare professionals working with them – there are so many at times it can be very confusing! Take the time to find out who they are and what they do.
Your team may consist of one or several of the following types of healthcare professionals, all aimed at supporting a different aspect of your recovery and rehabilitation. In many cases, you may see different people in the same role depending on the shift, time of week or their area of expertise. In addition, teaching hospitals like Vancouver General Hospital and GF Strong Rehab Centre also have medical and nursing trainees on staff who assist in care as part of their training.
Nursing Staff
The job of the nursing staff is to assist individuals with a spinal cord injury to attain and maintain maximum function. The nurses educate and assist individuals in adapting to an altered lifestyle, in collaboration with the rehabilitation team, while providing a therapeutic environment for client’s and their family’s development.
Social work (SW)
Physiotherapist (PT)
Occupational Therapist (OT)
Physiatrist (Physical Medicine and Rehabilitation)
Psychologist
A Psychologist provides evidence-based treatments to individuals with low mood, anxiety and other psychological challenges after SCI. Changes in sleep, chronic pain, mobility, accessibility and life roles are carefully considered in regards to their impact on psychological function. If there has been a change in thinking, memory and behaviour in addition to having a spinal cord injury the psychologist can help with assessing and treating these challenges together with the family and other team members.
Spine Surgeon
Recreation Therapist
Vocational Rehabilitation
Peer Coordinators
A peer coordinator is a person with a spinal cord injury who helps people with new injuries to understand how to live well after injury by building communities of support. Peer coordinators are knowledgeable about living with a spinal cord injury and share information about common challenges and successes.
Spinal Cord Injury’s Peer Support Program has regional coordinators across BC – you can find a Peer Coordinator in your area.
Outpatient/Spine Program Nurse
Assistive Technology
Clinical Dietitian
CONCLUSION
Spinal cord injury is caused by trauma or disease to the nerve pathways that connect the brain to the rest of the body. The location of the injury or lesion on the spinal cord determines the amount of the body affected. Spinal cord injury can cause partial or complete loss of mobility and sensation below the level of the injury, as well as affect the function of organ systems below the injury, however the spinal cord is rarely severed, and “completeness” of a spinal cord injury depends on whether there is any signal getting all the way to the bottom of the spinal cord. Each injury is unique, and it’s important that every person with spinal cord injury understands how their injury affects their body and participates in specialized rehabilitation.
RESOURCES
- SCI U – What is SCI? – A comprehensive video learning series on Spinal Cord Injury and its effects.
- Incomplete vs Complete – Further reading on incomplete vs. complete spinal cord injuries.
- ASIA Impairment Scale – American Spinal Injury Association Impairment Scale worksheet (for clinicians).
- Bowel Management – Jump to the LivingWithSCI.ca page on Bowel Management.
- Bladder Management – Jump to the LivingWithSCI.ca page on Bladder Management.
- Sexual Health – SCI-specific Sexual Health resource by the authors of LivingWithSCI.ca.
- Autonomic Dysreflexia – Jump to the LivingWithSCI.ca page on Autonomic Dysreflexia.
- Spinal Cord Injury Chronic Pain – Pain Management Network in New South Wales, Australia, featuring videos about SCI pain and an SCI Pain Navigator tool.
READ MORE
Four stories of epidural stimulation from The Spin.
This website contains general information about medical conditions and treatments. All information, content, and material of this website is for informational purposes only and are not intended to serve as a substitute for the consultation, diagnosis, and/or medical treatment of a qualified physician or healthcare provider. (c) 2024 Spinal Cord Injury BC
